What Causes Type 2 Diabetes?
Type 2 Diabetes is the most common type of Diabetes that is characterized by an individual’s body not properly using insulin as it should; as a result of this, the body is unable to compensate by producing enough insulin to replace the amount being used by the body. Type 2 Diabetes develops in individuals of all ages, but is often found in middle-aged and older individuals who are either overweight or obese.
What Causes Type 2 Diabetes?
Genetic Predisposition
When in person is born, they are passed on genes, or combinations of genes, from their biological mother or father. These genes can either increase or decrease ones likelihood of developing this type of Diabetes. It has been found, through research, that certain ethnicities are more likely to develop Diabetes; these ethnicities include African Americans, Hispanics, Alaska Natives,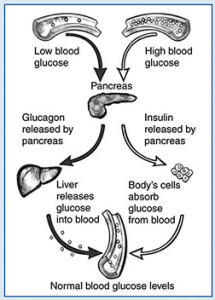 and more. It has also been discovered that there is a higher rate of Type 2 Diabetes in families and identical twins.
and more. It has also been discovered that there is a higher rate of Type 2 Diabetes in families and identical twins.
Studies have also determined gene variants increase the likelihood of developing this disease. Although the research is not fully complete and many gene variants are still unknown, scientists do know that genes have the ability of affecting insulin production in ones body. They also know that these genes do not affect insulin resistance.
One of the gene variants scientists have discovered that increase one’s likelihood of getting Type 2 Diabetes is the variant of the TCF7L gene. For those who have these gene variants, there is an 80% higher chance of developing the disease than those who do not carry the genes. Even though their risk is so high, there are things these people can do in order to delay the disease such as dieting, working out, and losing weight.
Another role that genes play in developing Diabetes is making one more likely or susceptible of becoming obese or overweight. There is a “Thrifty Gene” theory that states certain genes in one’s body increase metabolism which results in the body extracting energy from the food one eats and using it as energy in the future. Although this may be a good situation if you’re scarce or deprived of food, it is not an ideal situation for those who intake many high-calorie foods because it can lead to obesity, and in the end, Diabetes.
Obesity & Inactivity
 As stated above, obesity and being physically unfit is one of the main causes of Type 2 Diabetes. When someone continuously puts a lot of calories in their body, through the foods they eat, but does not do enough physical activity to burn those calories, a insulin resistance is created. Since insulin resistance is present in those with Type Two Diabetes; a person is more likely to develop it. Central obesity, which is defined as obesity associated with excess abdominal fat, puts one at risk of developing insulin resistance, diabetes, and heart and blood vessel disease. This negative affects to the body are caused the hormones that the excess fat on the stomach produce.
As stated above, obesity and being physically unfit is one of the main causes of Type 2 Diabetes. When someone continuously puts a lot of calories in their body, through the foods they eat, but does not do enough physical activity to burn those calories, a insulin resistance is created. Since insulin resistance is present in those with Type Two Diabetes; a person is more likely to develop it. Central obesity, which is defined as obesity associated with excess abdominal fat, puts one at risk of developing insulin resistance, diabetes, and heart and blood vessel disease. This negative affects to the body are caused the hormones that the excess fat on the stomach produce.
Studies have shown that those who are at risk due to this factor can decrease the risk by changing their lifestyle when it comes to food choices and physical activity routines. It has been proven that, by losing weight, regularly exercising, and eating a low-fat and low-calorie diet, can lower one’s risk significantly.
Insulin Resistance/Metabolic Syndrome
As stated above, those who are overweight or lacking physical activity can develop an insulin resistance, which increases the risk of developing Type 2 Diabetes. This is known as metabolic syndrome and is defined as a group of conditions that include high blood glucose levels, excess abdominal fat, high blood pressure, and abnormal levels of cholesterol and triglycerides in the blood.
When your muscles, liver, and fat stop responding to insulin effectively, the pancreas is pressured to produce extra insulin to compensate for the amount used. This can lead to Diabetes because if the beta cells in the body are not working properly, glucose in the blood stream rises. In order to reverse this syndrome, individuals can make some life changes such as getting more physical activity, eating healthy, and losing weight. These actions improve how the body responds to the levels of insulin.
Abnormal Glucose Production by the Liver
In some cases, individuals who have Diabetes have livers that produce an unhealthy amount of glucose. The way this works is through a hormones called glucagon that are released by the pancreas; this hormone stimulates the liver and produces the glucose that eventually finds its way into our blood steam.
Glucagon is typically released into the body with glucose and insulin levels are low, but after one eats, their levels are low which results in glucagon levels dropping and the liver storing additional glucose for when it is required.
Those who have Diabetes’ bodies are unable to lower their level of glucagon after a meal, which means their levels are higher than they should be; the liver then produces glucose that is not needed and the level of glucose in the blood is too high. As we know, increased glucose levels in the blood can contribute to Diabetes.
The Roles of Insulin and Glucagon in Normal Blood Glucose Regulation
One who is healthy is able to maintain their glucose levels by a variety of means. Insulin and glucagon work together to regulate these levels of glucose in the blood; insulin that is made by beta cells lowers glucose levels, and glucagon does the opposite.
The role that insulin and glucagon in normal glucose regulation may be confusing to some, but here is the breakdown of how it all works. Insulin helps our bodies absorb glucose from our blood, which results in lower levels of glucose; it also stimulate our livers and muscle tissue that store excess glucose.
Insulin lowers our blood glucose levels by reducing the amount that our livers produce; when we have low level of glucose, our pancreas releases glucagon and signals our liver and muscle tissues to break it down and turn it to glucose. This results in an increased level of glucose.
Cell Signaling and Regulation
The cells in our bodies connect with each other through molecular signaling pathways. One of the relative ways cells signal each  other in terms of diabetes is our insulin receptors capturing insulin molecules that are in our blood stream. When this communication is done, insulin and its receptor enable the cells in our bodies to absorb glucose and use or store it for energy. The issue will this signaling system is that some of the signals that are communicated, through the insulin signal cells, lead to inflammation and insulin resistance.
other in terms of diabetes is our insulin receptors capturing insulin molecules that are in our blood stream. When this communication is done, insulin and its receptor enable the cells in our bodies to absorb glucose and use or store it for energy. The issue will this signaling system is that some of the signals that are communicated, through the insulin signal cells, lead to inflammation and insulin resistance.
Beta Cell Dysfunction
Another factor that causes Diabetes is beta cell dysfunction; this dysfunction results in abnormal amounts of insulin in the body. Scientists have been working to find the causes of this dysfunction, but in most cases, it has not been found. What they have found, though, is a gene, that regulates insulin in beta cells. This can lead to diabetes in the young, but it is rare. Although rare, it gives insight as to how beta cell dysfunction may be caused.
Risk Factors Associated with Developing Type 2 Diabetes
There are a variety of risk factors associated with developing Type 2 Diabetes. Some of these risk factors include:
- 45 or older
- Overweight
- Family members who are diagnosed with the disease
- Certain ethnicities such as the one stated in the article above
- High blood pressure
- Physically inactive and unfit
These are just a few of the risk factors associated with Type 2 Diabetes. Others include giving birth to a child who weighs above 9 pounds, certain levels of cholesterol or triglyceride, polycystic ovary syndrome, and pre diabetes.

